Can Your #SunRegrets Put You At Risk For Nonmelanoma Skin Cancer?
What puts you at risk for nonmelanoma skin cancer (NMSC)?
What Are Your Sun Regrets?

BABY OIL

TANNING BEDS

Sunbathing
Sun worshiping might seem like the only way to get perfectly bronzed skin, but it can lead to some serious regrets. Spending any amount of time in the sun without proper sun protection can cause damage to your skin. Sunbathing for long periods of time can lead to sunburns, accelerated skin aging and even skin cancer.4,18

NO DAILY UV PROTECTION
We all know that we should be wearing sunscreen. But many of us don’t do it every day, even when we know we should. According to the Skin Cancer Foundation, sun damage to the skin’s DNA is cumulative, so even brief exposure without sun protection can add up over time.
Understanding the Signs of Nonmelanoma Skin Cancer
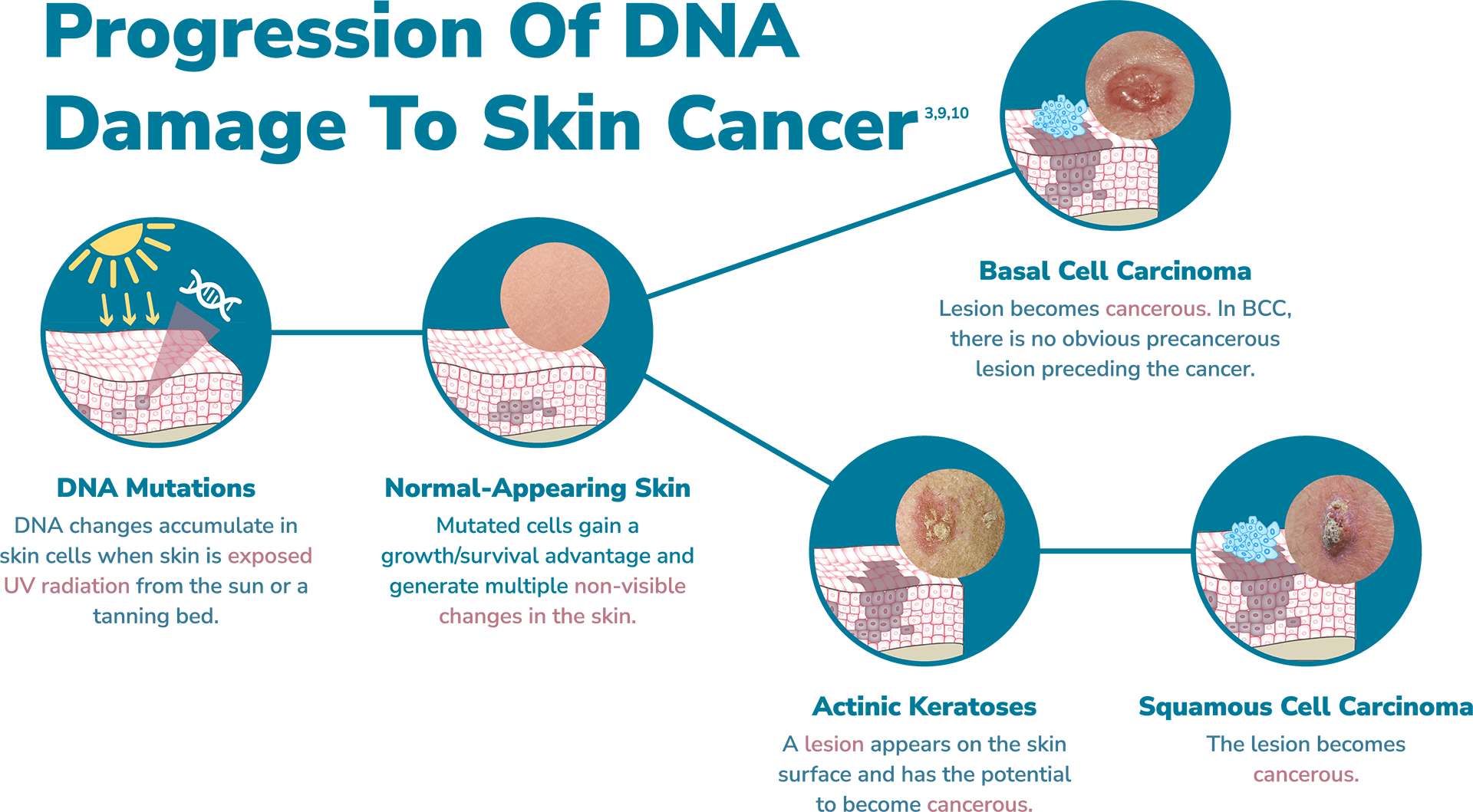
UV damage to the skin’s cells can lead to precancerous actinic keratosis (AK) or the two most common nonmelanoma skin cancers, squamous cell carcinoma (SCC) and basal cell carcinoma (BCC). Once the skin is exposed to UV rays, DNA mutations begin to accumulate in skin cells, generating multiple non-visible lesions beneath the skin’s surface. Over time, lesions can become visible on the surface of the skin and can progress into skin cancer.8 The good news is, when identified and caught early, NMSC is highly treatable.4
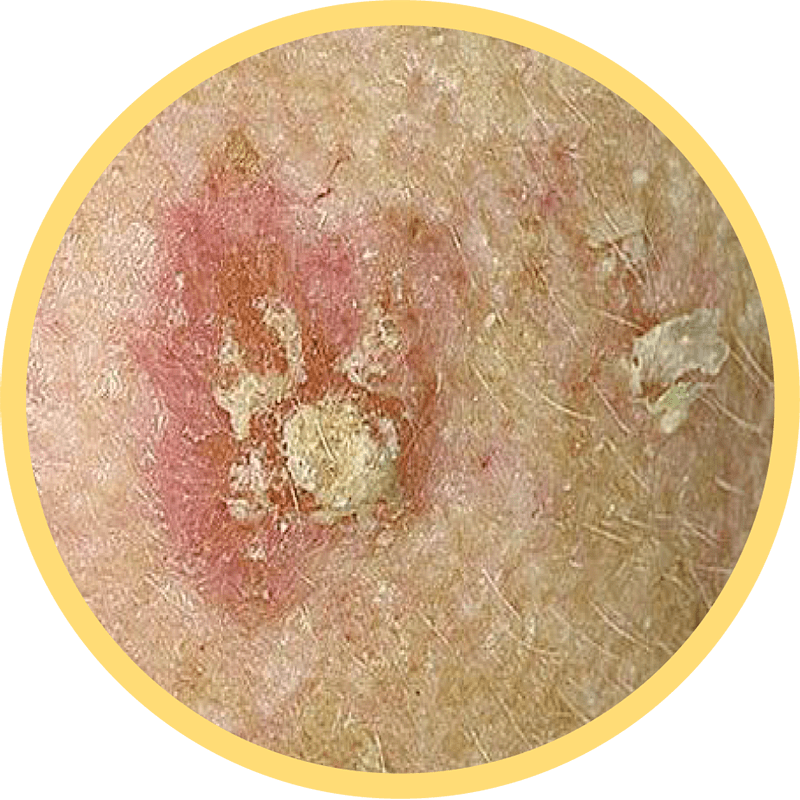

Actinic keratosis
The bumps may be raised or thick and may itch or have a sore feeling. AKs are most commonly found on the face, scalp, ears, back of the hands or chest, but can also appear on other sun-exposed areas of the body.12
Basal Cell Carcinoma
BCCs often look like red patches, pearly bumps on the sun-exposed areas of the body, such as the face, chest and back. They can also look like open sores, pink growths or scar-like areas.15
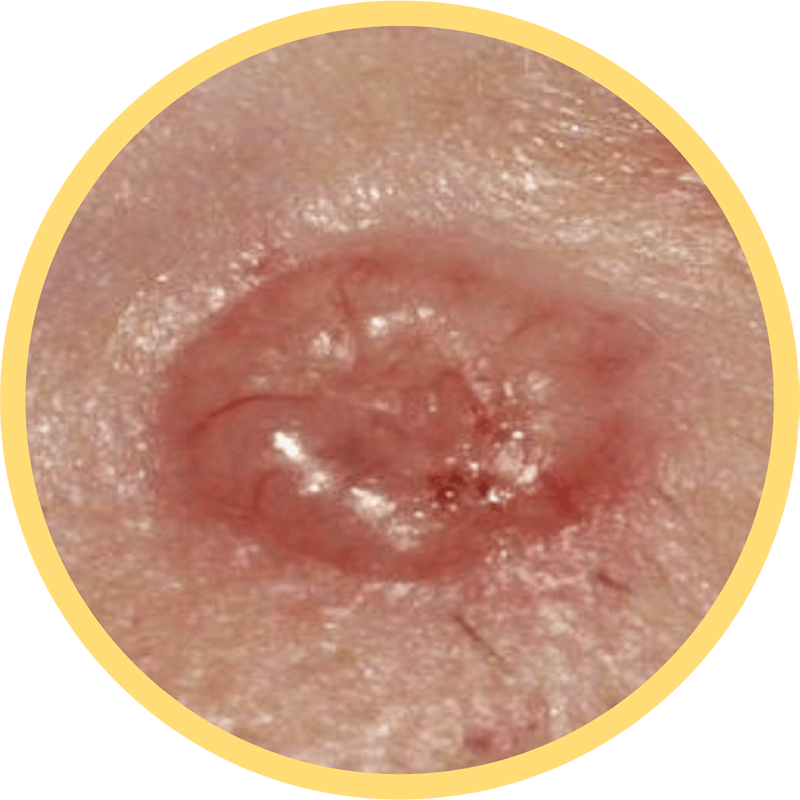
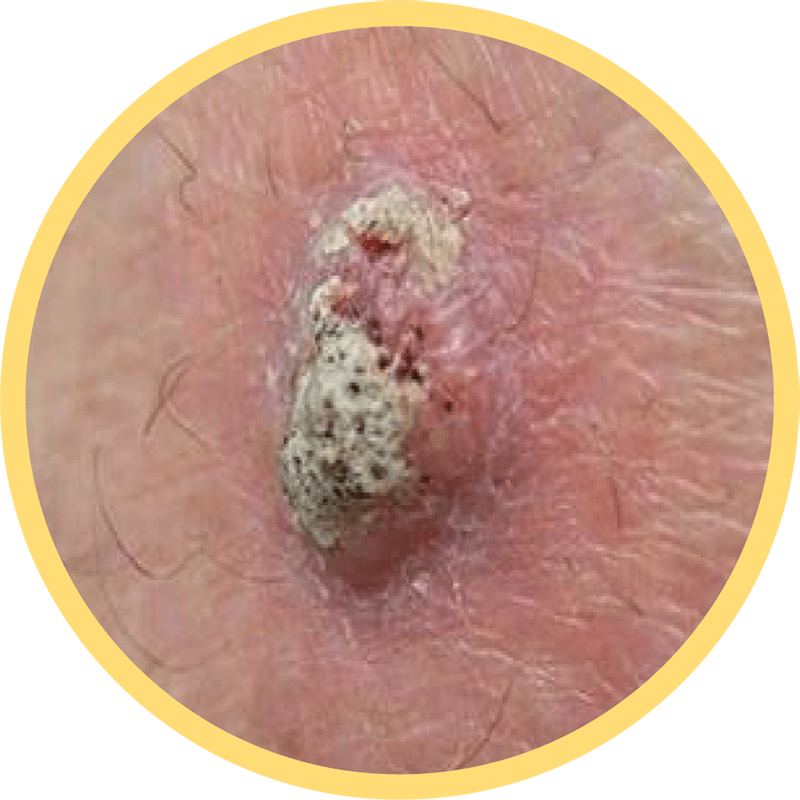

Squamous Cell Carcinoma
It typically appears as scaly red patches or firm red bumps or growths with raised edges and a lower center. SCC can also look like an open sore that doesn’t heal.17
Did You Know?
Scientists are researching how and if damage to the DNA of skin cells can be reversed or repaired. Currently, there are options to reduce the visual aspects of sun damage to the skin through topical treatments and procedures. Board-certified dermatologists may use and recommend retinoids, chemical peels, laser treatment and/or microdermabrasion.18
#SunRegrets Blog
What Your Skin’s DNA Can Tell You About Your Risk For Skin Cancer
Let’s understand what your skin’s DNA can tell you about your risk for developing skin cancer.
Learn About Nonmelanoma Skin Cancer
Learn about the risk factors and early detection of nonmelanoma skin cancer
Skin Cancer Myths
In this guide, we’ll debunk some of the most common skin cancer myths and give you information about how to protect yourself from this disease.
- Basic information about skin cancer. Centers for Disease Control and Prevention. https://www.cdc.gov/cancer/skin/basic_info/index.htm#:~:text=Basal%20and%20squamous%20cell%20carcinomas,Risk%20Factors%20for%20Skin%20Cancer%3F. Accessed November 18, 2022.
- Pleasance E.D., Cheetham R.K., Stephens P.J. A comprehensive catalogue of somatic mutations from a human cancer genome. Nature. Jan 14, 2010;463(7278):191–196.
- Young Kim, Yu-Ying He. Ultraviolet radiation-induced non-melanoma skin cancer: Regulation of DNA damage repair and inflammation. Genes & Diseases. Sept 16, 2014; 1(2); 188-189.
- American Cancer Society. Cancer Facts & Figures 2022. Accessed Feb. 23, 2023. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2022/2022-cancer-facts-and-figures.pdf
- Wu S, Cho E, Li WQ, Weinstock MA, Han J, Qureshi AA. History of Severe Sunburn and Risk of Skin Cancer Among Women and Men in 2 Prospective Cohort Studies. Am J Epidemiol. 2016 May 1;183(9):824-33.
- Nilsen LT, Hannevik M, Veierød MB. Ultraviolet exposure from indoor tanning devices: a systematic review. Br J Dermatol. 2016 Apr;174(4):730-40..
- Wehner MR, Chren MM, Nameth D, Choudhry A, Gaskins M, Nead KT, Boscardin WJ, Linos E. International prevalence of indoor tanning: a systematic review and meta-analysis. JAMA Dermatol. 2014 Apr;150(4):390-400.
- Huang, A.H., Chien, A.L. Photoaging: a Review of Current Literature. Curr Derm Rep 9, 22–29 (2020). https://doi.org/10.1007/s13671-020-00288-0.
- Xiang F, Lucas R, Hales S, Neale R. Incidence of nonmelanoma skin cancer in relation to ambient UV radiation in white populations, 1978-2012: empirical relationships. JAMA Dermatol. 2014 Oct;150(10):1063-71.
- Huang A, Nguyen JK, Austin E, Mamalis A, Jagdeo J. Updates on Treatment Approaches for Cutaneous Field Cancerization. Curr Dermatol Rep. 2019 Sep;8(3):122-132.
- American Academy of Dermatology. Actinic Keratosis: Overview. Accessed Nov. 16, 2022. https://www.aad.org/public/diseases/skin-cancer/actinic-keratosis-overview
- American Academy of Dermatology. What are the signs and symptoms of actinic keratosis? Accessed Feb. 23, 2022. https://www.aad.org/public/diseases/skin-cancer/actinic-keratosis-symptoms
- Neugebauer R, Levandoski KA, Zhu Z, Sokil M, Chren MM, Friedman GD, Asgari MM. A real-world, community-based cohort study comparing the effectiveness of topical fluorouracil versus topical imiquimod for the treatment of actinic keratosis. J Am Acad Dermatol. 2018 Apr;78(4):710-71.
- American Cancer Society. Key statistics for basal and squamous cell cancers. Accessed Nov. 8, 2022. https://www.cancer.org/cancer/basal-and-squamous-cell-skin-cancer/about/key-statistics.html.
- American Academy of Dermatology. Skin Cancer Types: Basal Cell Carcinoma Signs and Symptoms. Accessed Feb. 23, 2022. https://www.aad.org/public/diseases/skin-cancer/types/common/bcc/symptoms
- American Cancer Society. What are Basal and Squamous Cell Skin Cancers. Accessed Nov. 9, 2022. https://www.cancer.org/cancer/basal-and-squamous-cell-skin-cancer/about/what-is-basal-and-squamous-cell.html
- American Academy of Dermatology. Skin Cancer Types: Squamous Cell Carcinoma Signs and Symptoms https://www.aad.org/public/diseases/skin-cancer/types/common/scc/symptoms
- American Academy of Dermatology. How Dermatologists Treat Sun-Damaged Skin. https://www.aad.org/public/everyday-care/sun-protection/sun-damage-skin/wrinkles-sun-damage-can-be-treated. Accessed 12/2/2022.